 Ask family members, visitors, and care providers to stay home if they are sick. Education of patients, families, visitors, and care providers about how respiratory infections are transmitted and how respiratory illness can be prevented.These measures are part of the standard precautions that should be taken to prevent the spread of disease. Respiratory hygiene and cough etiquette are infection prevention measures to decrease the transmission of respiratory illness such as influenza or cold viruses in healthcare facilities where patients, employees, and visitors may not be immediately recognized as having a respiratory infection. Healthcare workers should not eat or drink in isolation rooms and should always clean their hands before entering the room and upon exiting the room. All healthcare workers and visitors need to follow these guidelines. Generally, when patients are placed on isolation precautions, there will be a sign at the door of their hospital rooms to remind visitors and healthcare workers which isolation precautions are needed. These precautions protect patients, families, visitors, and healthcare workers from the spread of germs. Isolation precautions are used to help stop the spread of germs from one person to another. Safe handling of potentially contaminated equipment or surfaces in the patient environment, and.Use of personal protective equipment (e.g., gloves, gowns, masks).If an airborne infection isolation room is not available, aerosol-generating procedures may still be safely performed as long as the providers are wearing appropriate respiratory personal protective equipment, extra attention is paid to keeping the doors closed, and reentry without airborne precautions does not occur until the time needed to ensure at least 99% removal efficiency, based on air exchanges per hour for each room as determined by hospital engineering.Standard precautions are the minimum infection prevention practices that should be used in the care of all patients all of the time. These practices are designed to both protect the healthcare worker and to prevent the healthcare worker from spreading infections among patients. If providers are performing an aerosol-generating procedure for a patient with known or suspected COVID-19, we recommend that they take the same airborne and contact precautions whether or not the procedure occurs in an airborne infection isolation room. Our greatest concern about this misconception is that providers will use insufficient personal protective equipment precautions or withhold essential treatments because such a room is not available. If the patient is continuously generating aerosolized particles, as occurs with normal breathing without a mask, coughing, or ongoing noninvasive respiratory support, negative pressure and air exchanges will not make the room much safer, especially if one is close to the patient. 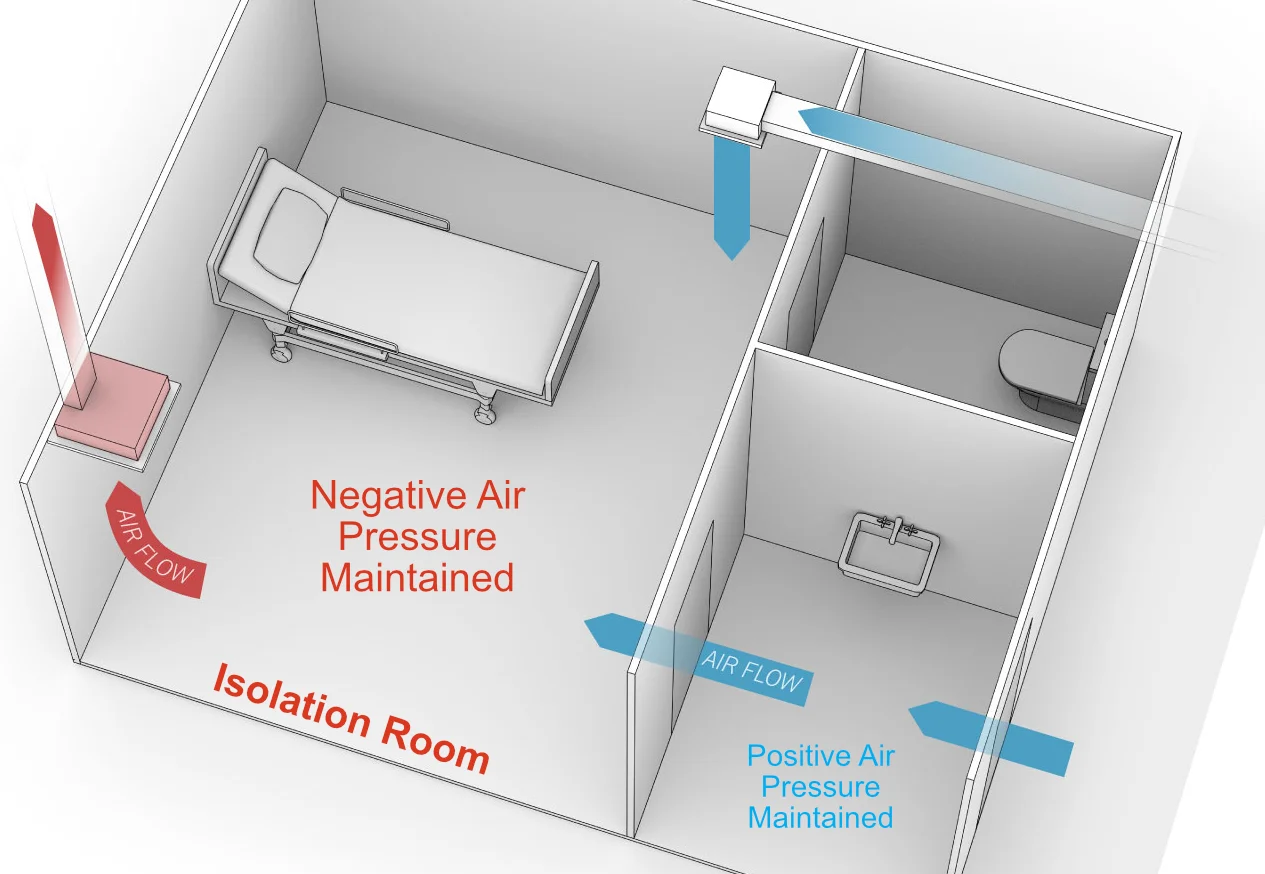
1 Even with enhanced air exchanges in airborne infection isolation rooms, we have no evidence that physicians, nurses, or respiratory therapists performing an aerosol-generating procedure are protected in any way. For comparison, a standard patient room with 6 air exchanges per hour requires 69 minutes for 99.9% efficiency. 
Twelve air exchanges per hour is recommended for an airborne infection isolation room, meaning 23 minutes is required for 99% air removal efficiency and 35 minutes for 99.9% efficiency. They help protect individuals outside the room by keeping more aerosol within the room when the doors are opened and offer the benefit of enhanced air exchanges, which reduces the time from completion of an aerosol-generating procedure until it is safe to reenter the room without complete airborne personal protective equipment precautions. Unfortunately, these rooms do little to protect individuals in the room with the patient during the aerosol-generating procedure. 2 Many of our colleagues believe this is endorsed because they are safer in such a room. In its zeal to protect health care professionals, the Centers for Disease Control and Prevention recommends that aerosol-generating procedures, such as noninvasive positive-pressure ventilation and intubation, “ideally” be conducted in an airborne infection isolation room. 
The preferred terminology is airborne infection isolation room, which is defined as having negative pressure, 6 to 12 air exchanges per hour (12 preferred), and direct exhaust to the outside or through a high efficiency particulate air filter. We would like to shed light on a common yet dangerous misperception in the medical community about so-called negative-pressure rooms. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
